马上注册,阅读更多内容,享用更多功能!
您需要 登录 才可以下载或查看,没有账号?立即注册 
×
Comparative Outcomes of Redo and Initial Tracheal Resection and Anastomosis: A 25-Year Experience with Insights from a Propensity Score-Matched Analysis
Objective: We aimed to compare the outcomes of tracheal resection and anastomosis (TRA) between patients undergoing initial TRA (iTRA) and those undergoing redo TRA (reTRA).
Methods: In this retrospective cohort study, we used our prospectively collected database of patients with laryngotracheal stenosis treated at our tertiary thoracic surgery center over the past twenty-five years. Patients who underwent TRA between March 2000 and March 2025 were included. We excluded operations performed for tracheal tumors, multi-segmental stenosis, tracheoesophageal fistula, and those lost to follow-up. A total of 1,465 patients were included, of whom 49 had a history of TRA at another center and 36 had both their initial and redo TRA at our institution, yielding 85 reTRA and 1,416 iTRA cases. Postoperative complications and outcomes were compared. To ensure a robust comparison, propensity score matching (PSM) was performed, resulting in 71 matched pairs of iTRA and reTRA patients.
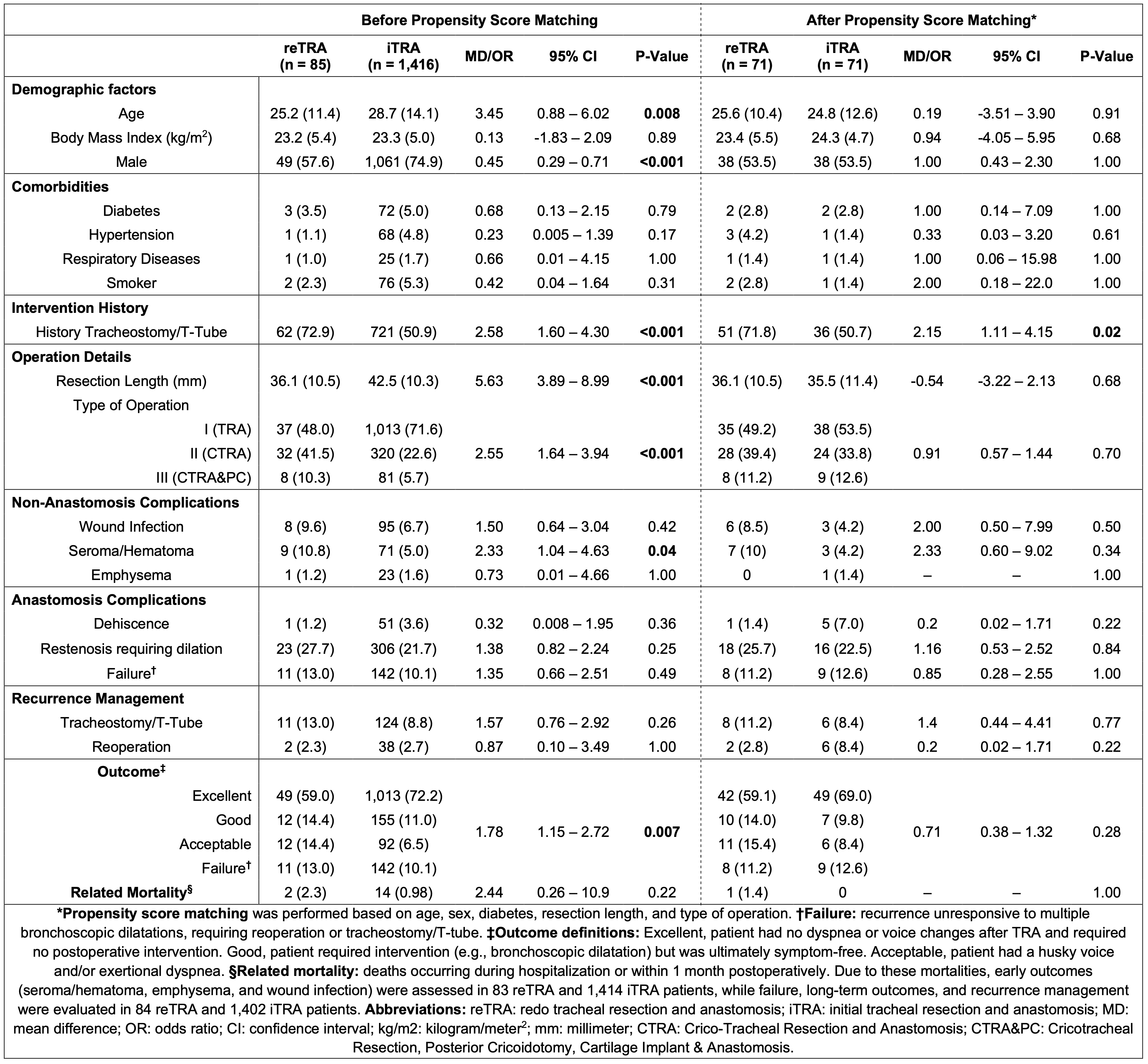
Results: Before matching, the two groups differed significantly in age, gender, resection length, and type of operation. These differences were balanced after PSM. Comorbidities were similar both before and after matching. As shown in Table 1, among 84 reTRA and 1,402 iTRA cases, postoperative outcomes were better in the iTRA group before matching, with a higher rate of excellent outcomes (72.2% vs. 59.0%; odds ratio [OR] 1.78, 95%confidence interval [CI] 1.15–2.72, p-value = 0.007). However, this difference was no longer significant after PSM (OR 0.71, 95%CI 0.38–1.32, p-value = 0.28). Failure rates were comparable between initial and redo surgeries (10.1% vs 13.0%, p-value = 0.70) and remained similar after matching (12.6% vs 11.2%, p-value = 1.00), as well. There were no significant differences between the groups, before or after matching, in the rates of subcutaneous emphysema, wound infection, dehiscence, or postoperative required bronchoscopic dilatations. The only notable difference was a higher incidence of seroma/hematoma in the reTRA group before PSM, (9 [10.8%] vs 71 [5.0%], OR 2.33, 95%CI: 1.04–4.63, p-value = 0.04), which was not observed after PSM (7 [10.0%] vs 3 [4.2%], OR 2.33, 95%CI: 0.60–9.02, p-value = 0.34).
Conclusions: Redo tracheal resection and anastomosis is not necessarily associated with higher rates of failure, complications, or poor outcomes. Although technically more challenging, redo TRA could be performed safely with comparable outcomes to initial TRA.
Arman Hasanzade (1), Fariba Ghorbani (1), Amir Ali Mahboobipour (1), Salman Soleimani (2), Mahboubeh Asadi (1), Azizollah Abbasi Dezfouli (2), Mohammad Behgam Shadmehr (1), (1) Tracheal Diseases Research Center, National Research Institute of Tuberculosis and Lung Diseases, Shahid Beheshti University of Medical Sciences, Tehran, Tehran, (2) Lung Transplantation Research Center, National Research Institute of Tuberculosis and Lung Diseases, Shahid Beheshti University of Medical Sciences, Tehran, Tehran
|