马上注册,阅读更多内容,享用更多功能!
您需要 登录 才可以下载或查看,没有账号?立即注册 
×
Operationalizing Limited Resection: Left Upper Tri-segmentectomy vs Lobectomy for Occult N+ Stage I NSCLC
Objective: While retrospective studies suggest comparable efficacy between left upper lobectomy (LUL) and left upper tri-segmentectomy (LUTS) for stage I left upper non-small cell lung cancer (NSCLC), it remains unclear whether this equivalence holds for patients found to have occult nodal metastasis (pathologically upstaged to N1/N2). This study compares the perioperative and long-term oncological outcomes of LUL and LUTS in patients with clinical stage I disease who were subsequently found to have occult lymph node disease.
Methods: This study included stage I patients who underwent LUL or LUTS between August 2014 and November 2023 and were pathologically upstaged for lymph node status (N1/N2). Patients had tumors located at least 2 cm from the lingular segment. Propensity score matching (PSM) was used to address baseline imbalances between groups. Perioperative outcomes, overall survival (OS), recurrence-free survival (RFS), lung cancer-specific survival (LCSS), and subgroup analyses were assessed.
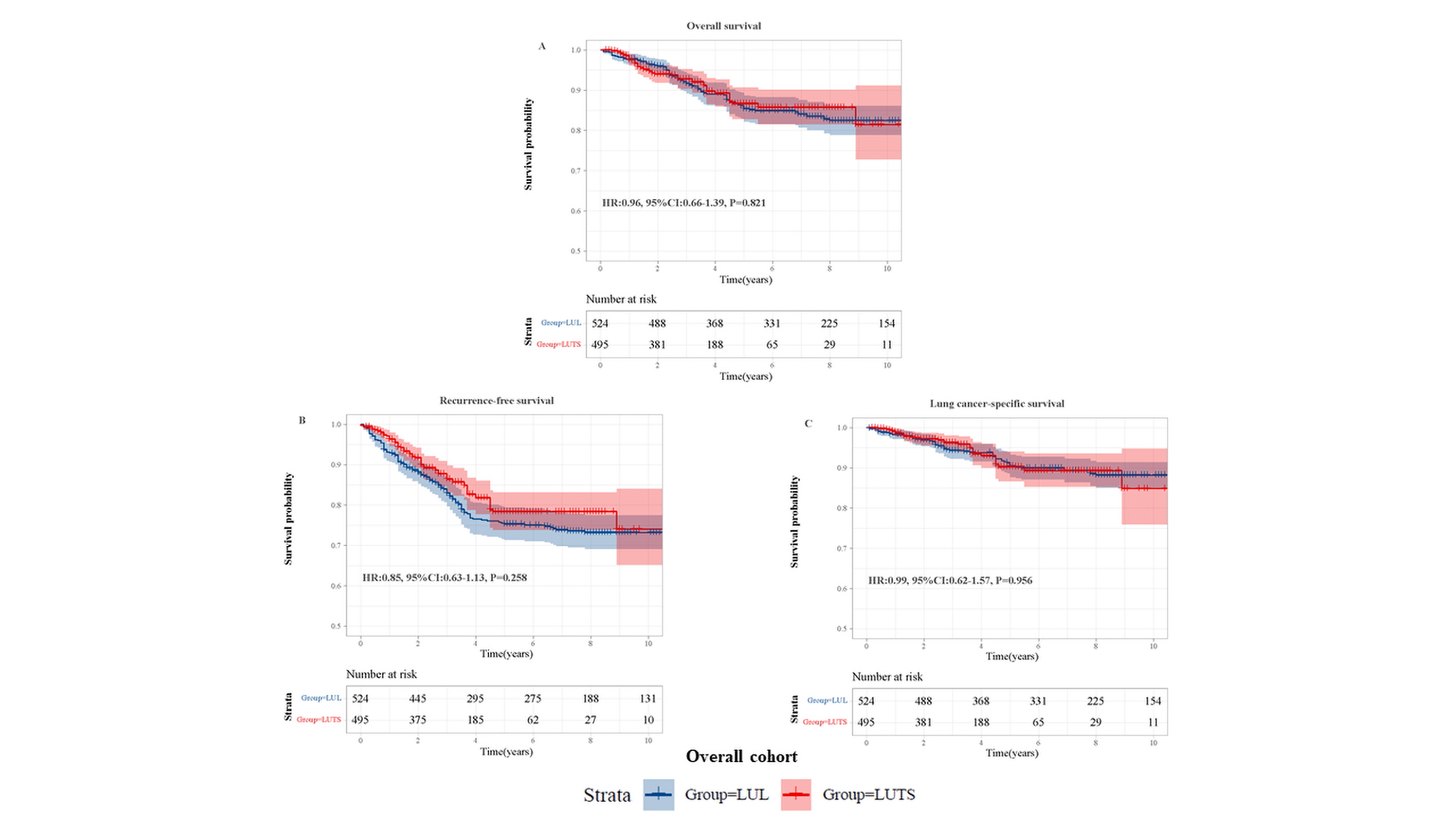
Results: A total of 1019 patients were included (LUL: 524; LUTS: 495) with a median follow-up of 4.8 years (IQR: 2.5-8.1). Occult N1 disease was present in 533 patients (52.3%) and occult N2 disease in 486 patients (47.7%). Compared to LUL, LUTS was associated with significantly shorter operative times (103 vs. 120 minutes, p=0.001), reduced postoperative drainage volume at 3 days (335 vs. 485 ml, p=0.001) and total drainage (360 vs. 530 ml, p=0.001), lower conversion to thoracotomy rates (1.0% vs. 3.4%, p=0.009), and fewer postoperative complications (9.9% vs. 14.9%, p=0.016). No significant differences were observed in 5-year OS (70.2% vs. 71.3%, HR: 0.96; 95% CI: 0.66-1.39; p=0.821), 5-year RFS (68.4% vs. 65.3%, HR: 0.85; 95% CI: 0.63-1.13; p=0.258), or 5-year LCSS (76.7% vs. 75.4%, HR: 0.99; 95% CI: 0.62-1.57; p=0.956) between the two groups.
Conclusion: For patients with stage I left upper NSCLC found to have occult nodal metastasis after resection, LUTS, while preserving adequate surgical margins, achieves superior perioperative outcomes and comparable long-term oncological results compared to LUL.
Zhang-Yi Dai (1), Jia-Jun Cheng (2), Fuqiang Wang (1), Xingqi Mi (3), Yikai Xing (1), Yafei Xie (1), Pengfei Ji (4), Yun Wang (4), (1) West China Hospital, Sichuan University, Chengdu, Sichuan, (2) Sichuan University West China Hospital, Chengdu, China, (3) West China Hospital, Sichuan University, Chengdu, Sichuan 610041, China, China, (4) West China Hospital, Sichuan University, Chengdu, NA
|